Categories
Detecting & Diagnosing Infertility
Nov 24, 2022
A thorough evaluation is an important aspect of the diagnosis of infertility and its subsequent treatment and management. Both partners should undergo evaluation simultaneously, although, most of the male partners prefer to be evaluated only after the female partner has been evaluated – this practice isn’t most advisable. Given that today male infertility is on the upswing and that both partners are equally at risk of being infertile it is it is essential to evaluate both partners together.
Some of the common evaluation procedures employed are enumerated below:
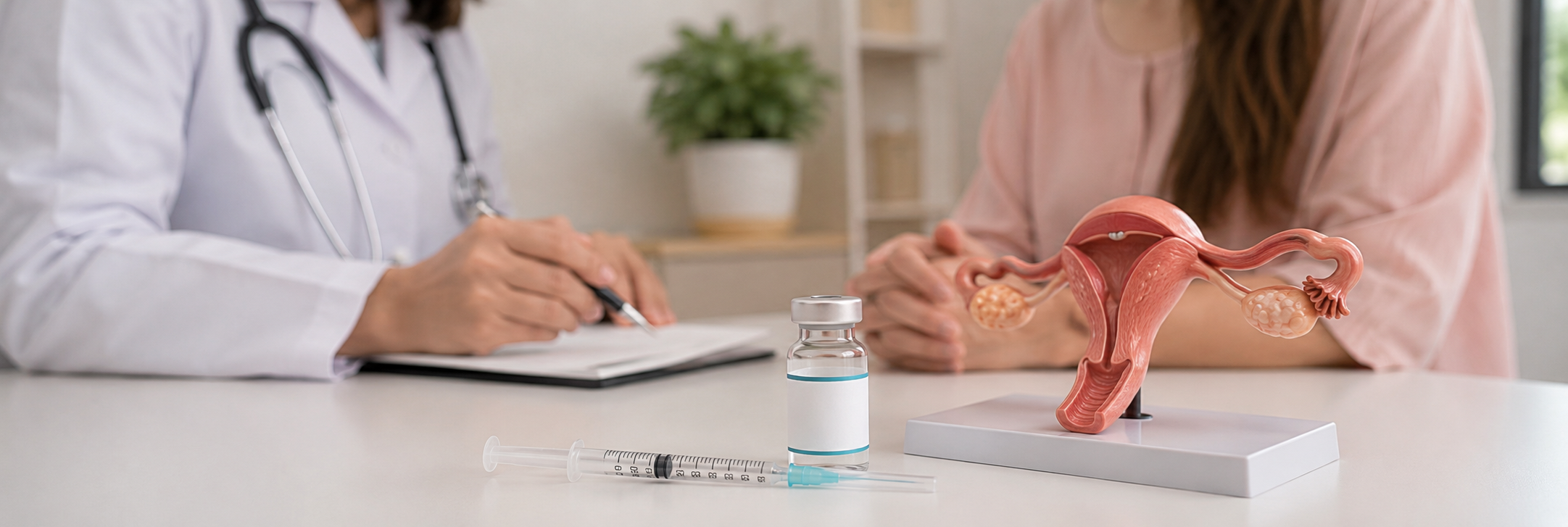
Evaluation of Female Infertility
The basis of any evaluation is the study of the basic medical history and a thorough physical examination followed by some preliminary tests. The evaluation takes into account the history of menstrual cycles and any known gynecological problems. Physical examination looks out for excessive hair growth and other physical manifestations which could suggest hormonal imbalances or anatomical factors.
Basic investigations that are employed include – ascertaining blood sugars; cervical smears and serology (HIV, HbsAg, VDRL, HCV). Hormonal tests such as FSH LH estradiol are carried on the second day of the menstrual cycle to rule out hormonal imbalances and identify any factors that can point to possible early menopause. Investigations also look to ascertain thyroid and prolactin malfunction, if any. Some of the other basic tests include:
1. Pelvic Ultrasound: A baseline ultrasound scan is performed to diagnose congenital anomalies of the reproductive tract, uterine, pelvic and other ovarian problems. The ovarian reserve is also assessed by measuring the number of eggs in the ovaries. A baseline follicular monitoring is also carried out to track ovulation.
2. Hysterosalpingography (HSG): HSG is the most common tool to assess the uterine cavity and patency of the fallopian tubes. This examination is performed after cessation of menses, and the couple is requested to avoid intercourse from the time of menstruation to the time of examination; this is to prevent interference with an early pregnancy demonstrated with HSG.
Following the above preliminary investigations, further evaluation and surgical treatment is ascertained based on their results. The following procedures could be employed as appropriate:
1. Hysteroscopy: Hysteroscopy is a simple procedure to visualize the cervical canal and the inside of the uterus using a thin, lighted, flexible tube - hysteroscope. The device is inserted through the vagina and can be used as both diagnostic and therapeutic tool - to remove a polyp, fibroid, adhesion or for biopsy
2. Laparoscopy: A laparoscopic visualization of the pelvic cavity is necessary to ascertain tubal patency, adnexal adhesions, and ovarian mass. Some abnormalities detected during the diagnostic laparoscopy can be treated during the same procedure - lysis of adhesions, salpingectomy, ovarian cystectomy, cauterization or vaporization of endometriotic implants. This procedure is performed under general anesthesia.
Evaluation of Male Infertility
Normal sperm count for a healthy male is measured at >15million/ml, however as much as the count the quality of the sperms is an equally important the determinant of male infertility.
Following a thorough check on the clinical history of the patient and a physical examination by the Andrologist, semen analysis is the first and foremost investigation performed to ascertain male infertility. In this preliminary assessment, certain physical characteristics like volume or quantity of the ejaculate are noted. While a microscopic examination helps measure the sperm count or the concentration; motility of the sperm (forward); morphological characteristics of the sperm (size and shape). This basic analysis forms the guide to further investigations and appropriate management.
If there are abnormalities detected in semen analysis, further evaluation is mandatory in the form of hormonal tests, doppler evaluation of the testis, transrectal ultrasound, and genetic tests. A complete absence of sperm in the in the semen calls for further investigations to understand the possible causes - decreased sperm production or impaired sperm transport due to a block in the ducts (Vas deferens).
General health investigations - blood sugars, cholesterol are also important factors in determining male infertility.